


Dr. Costello is now seeing patients in her new office location at
3915 Bristol Hwy, Suite 103, Johnson City, TN 37601
Office phone: 423-461-0073
Office fax: 423-461-0076
Now Scheduling weekdays by appointment only.
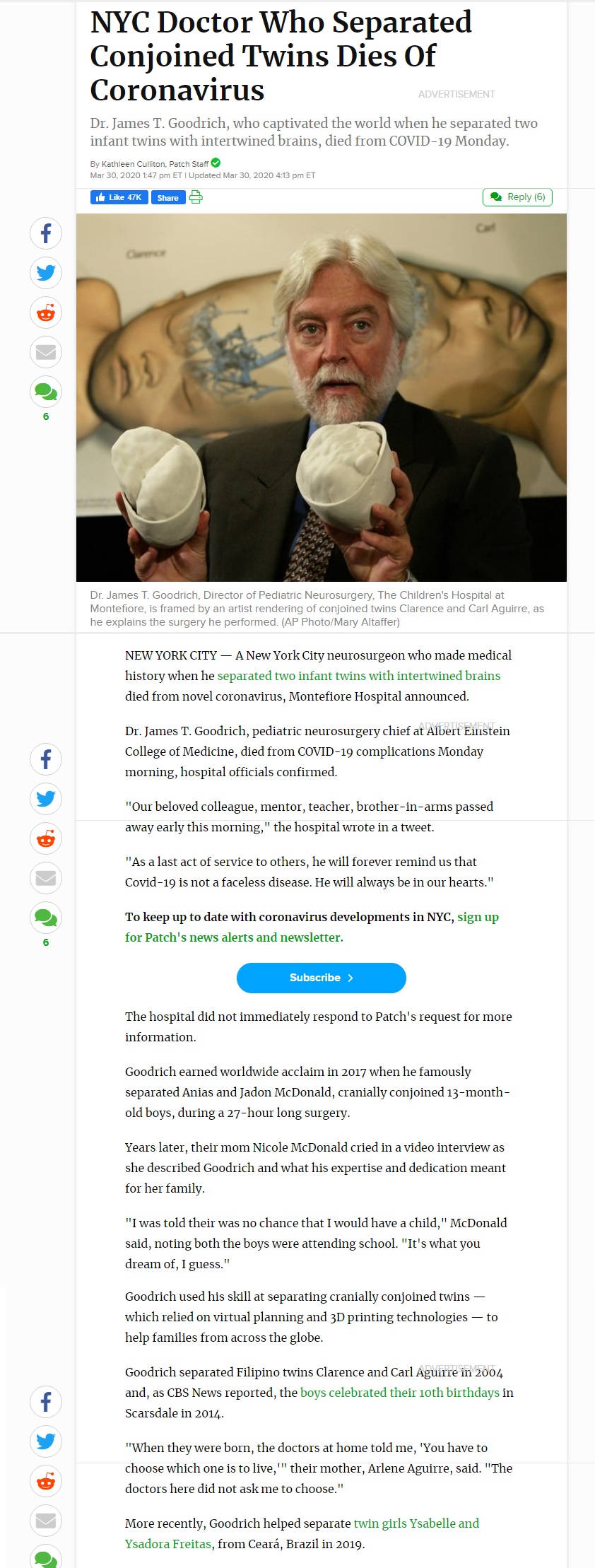
This was my dear professor, friend and mentor in NYC.
Thank you for everything you have done for the medical field.
In Memorium
Please watch this video about the conjoined twins on YouTube, link below
Montefiore – Neurological Surgery: Courage beat the odds
Link to article
NYC Doctor Who Separated Conjoined Twins Dies Of Coronavirus
Understanding the Environmental Influences of Neurotoxins on Your Brain: Fluoride
by Pamela Costello MD PC
A physician is obligated to consider more than a diseased organ, more even than the whole man — he must view the man in his world.
– Harvey Williams Cushing (1869-1939), Father of Neurosurgery
In my practice of holistic neurological medicine and surgery, I help patients identify and repair those issues causing damage or inflammation to their nervous and immune systems. That list can include potential structural issues, dietary stressors to the immune and nervous systems, infectious issues, as well as the exposure to an evergrowing list of environmental neurotoxins.
Added to the list is fluoride, which is indeed a neurotoxin. Extensive research studies dating back to the 1930’s* have shown its direct toxic effects on the central nervous system, as well as fluoride’s role in potentiating other neurotoxic heavy metals, such as Uranium, Lead, Aluminum, and Arsenic.
Fluoride is an environmental toxin that has absolutely no physiologic function in the body (only that of a poison/toxin), is sourced largely from industrial waste, and bioaccumulates in our bodies. We have no natural ability to excrete this toxin, therefore it accumulates in our tissues. Assessing the deleterious health risks of our exposure to fluoride must necessarily address the damage done by its accumulation from long term exposure.
In identifying and defining what is acting to poison our nervous systems, we can better understand and treat the escalating epidemics of neuroinflammatory illnesses. Fluoride added to our water or used as a dental treatment acts as a direct neurotoxin, potentiates the adverse effects of many other neurotoxins, and disables our cellular enzymatic systems. The known toxicity of this poison is sufficiently well established* to avoid
it in dental treatments, including as a drinking water additive.
We can no longer afford to ignore the issue as to what ends up in our air, water, food, and subsequently our brains. Adverse neuroimmunologic reactions to processed foods and their chemical contaminants, to indoor and outdoor air pollution with petrochemicals and radiation, have become epidemic. Such reactions are being misdiagnosed by mainstream medical practitioners, and therefore not treated effectively. We see these
reactions as epidemic rises in neuroinflammatory illnesses from autism to MS, ALS, dementias, the full spectrum of cognitive dysfunction, neuropathies, intractable pain syndromes and, developmental and attentional dysfunction in children and cognitive and mood dysfunction in adults.
In the seventies, we learned just how bad Lead was for us after having been exposed to it for more than fifty years. Now we’re adding silicofluoride to the tap water which, in the developing fetus, acts to draw lead into their bodies, concentrating in their brains and bones. In developing children and adults, fluoride bioaccumulates in the tissues and wreaks havoc on a multitude of enzymatic and cellular processes. You can measure these toxic elements in diseased bones, brains and bodies. (And I do, on every patient in my practice).
There is a multitude of sources of toxic fluoride, from toothpastes and dental treatments, to our fluoridated tap water, to additives in soft drinks, etc. Identifying what you’re consuming at all times has become imperative, as you often do not excrete the toxic components, nor absorb the healthful ones. Your brain and body serve as the store houses, as these toxins prematurely age and damage your nervous and immune system, as well as the body.
Once aware of the underlying causal link of environmental toxin to neuroinflammatory illness, what comes next? The next step is to identify your toxic burden, and become aware of those sources of greatest exposure, then find qualified care in the remediation of your burden and any damage done to your health.
*Please see my links section for a fluoride toxicity reference list.
If you’d like a brain health/neurotoxin burden evaluation and an individualized, comprehensive treatment protocol, please contact my office at 505-503-8325.
I am very sorry to announce the closing of my practice here in Albuquerque, New Mexico as of end of business day December 27, 2018.
Please inquire by phone at 505-503-8325 with any questions you may have. Please consult with your primary care physician and/or your insurance carrier regarding alternative treating practitioners.
Further practice announcements/information will be provided when available on this website, so please follow me here to receive them.
I apologize for any inconvenience this may present to you and your healthcare
Dr. Pamela Costello MD PC
I would like to thank you for entrusting me and allowing me to provide you with medical care.
You must be logged in to post a comment.